The importance of mental health on overall well-being has been reflected in recent United States laws and regulations, starting with the 2008 Mental Health Parity and Addiction Equity Act, which required insurers to offer the same level of coverage for mental health treatment as for physical health.
Despite this growing understanding, research shows that while 20% of all people deal with mental health problems, only 30% of those individuals receive treatment for those issues. This is in part due to gaps in traditional care models, which can keep treatment difficult to access for certain groups, and lingering cultural stigmas around seeking help.
As a response, regulations around different mental healthcare services are changing, and mental health organizations are receiving more funding to support digital solutions to make mental healthcare more accessible and improve operations for mental health services organizations.
As the healthcare industry invests in digital transformation across internal operations and patient care, mental health service providers are following suit.
In this article, we’ll explain why digital transformation has become critical for the future of mental health services and how digital adoption platforms (DAPs) like Whatfix can strengthen providers’ digital transformation initiatives.
The Role of Digital Transformation in Mental Health Services
During COVID-19, the healthcare sector faced immense pressure to create virtual tools and resources as alternatives and supplements to in-person care. This led to a surge in mental health mobile apps, digital therapy programs, and asynchronous video, audio, and text communications between clinicians and patients.
This created a new landscape that allows providers to enhance and supplement in-person care with 24/7 access to personalized virtual support, bridge accessibility gaps, and equip patients with essential tools for proactively managing mental health.
Behind the scenes, mental health services providers also engage in digital transformation projects to optimize and streamline internal operations and recordkeeping processes. By utilizing new technologies to automate processes and facilitate virtual care, mental health services providers can dramatically expand their capacity to help patients while improving team member experience.
Key Technologies Powering Mental Health Services Transformation
In recent years, the mental healthcare sector has seen great digital innovation and disruption, and empowered providers with new ways to optimize everything from appointment scheduling to recordkeeping to diagnostics.
Here are some of the most influential digital technologies in mental healthcare today.
1. Teletherapy and virtual care platforms
The COVID-19 pandemic created an urgent need for new approaches to delivering telehealth services on a massive scale. This led to the development of new applications that allow organizations to offer real-time video sessions, asynchronous therapy, and digital patient scheduling.
2. AI for personalized care
AI is already playing a meaningful role in how providers tailor care to individual patients. Tools powered by machine learning can help clinicians track symptoms over time, flag patterns that may require intervention, and even recommend treatment adjustments. While still evolving, these capabilities give providers new ways to personalize care plans and improve outcomes at scale.

3. Mobile mental health apps and self-guided programs
Not every patient needs or has access to ongoing clinical therapy, which has fueled the growth of mobile apps and self-guided programs. From CBT-based tools to meditation apps and mood trackers, these solutions empower people to manage aspects of their mental health on their own terms. For providers, they also offer a way to extend support beyond traditional care settings and reach underserved populations.

4. EHR and interoperability improvements
Digital transformation in mental health services also extends to service provider operations. By investing in modern EHR software and other general operational applications, providers can streamline workflows more efficiently and facilitate inter-facility transmission of documentation and records for better coordinated care and outcomes tracking.

Barriers to Digital Transformation in Mental Health Services
Implementing new technology in healthcare settings is uniquely challenging. The sensitive nature of mental health creates an intense need for continuity of service through change management and training activities.
Here are some of the most common digital transformation challenges seen by mental healthcare organizations:
- Data Security and Privacy Compliance: Protecting patient data is non-negotiable in mental health services. Every new system has to meet HIPAA, GDPR, and other evolving standards, which limits vendor options and drives up costs. That reality often slows down transformation compared to other industries.
- Digital Literacy and Access Gaps: Not everyone (clinicians, staff, or patients) uses new technology with the same comfort level. Patients in particular may face digital literacy challenges and the stress of managing their care, making adoption harder. Leaders need training and support strategies that make tools accessible for all groups.
- Clinician Resistance and Burnout: Change fatigue is real, especially when multiple initiatives roll out simultaneously. Without the right change management approach, clinicians can become disengaged, burned out, or revert to old processes. Transformation works best when adoption is paced and supported with clear benefits for staff.
- Disconnected Tech Stacks: Budgets often force organizations to implement tools one at a time, but without integration, systems like EHR, billing, and telehealth quickly become silos. That fragmentation adds friction for both providers and patients. Long-term success depends on building a connected, interoperable tech ecosystem.
How DAPs Accelerate Transformation
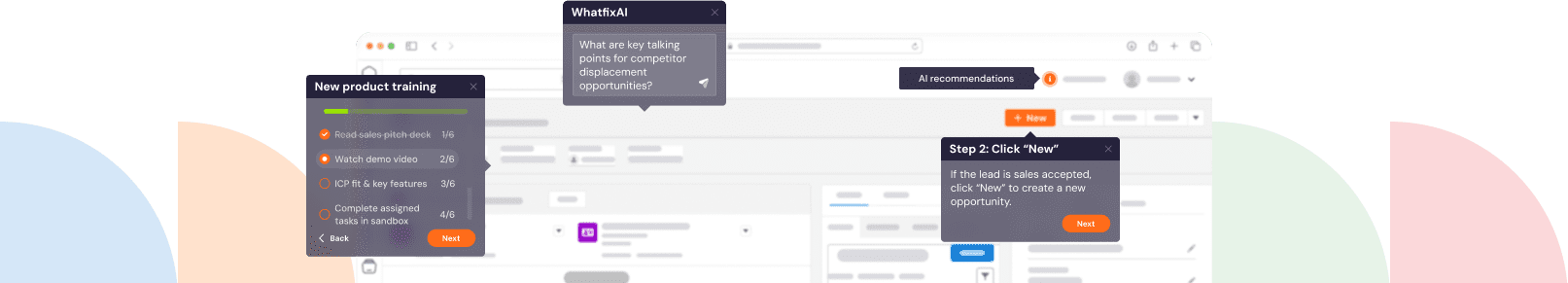
A digital adoption platform (DAP) is an enterprise software that creates and delivers information to end-users via messages, in-app guidance, embedded support, and other help widgets that sit on top of the daily applications employees and patients interact with, from scheduling portals to EHR platforms.
With a DAP, IT teams and managers can create role and event-specific tips, tutorials, and links to self-help resources that can be deployed at relevant times within the user journey as support. This accelerates patient portal onboarding, supports healthcare workers in the flow of work, and contextualizes experiences depending on the end-user (physician, patient, admin staff, nurse), making the difference between successful and failing digital transformation projects.
In a mental healthcare context, these features allow providers to deliver personalized training activities that let users learn in the flow of a particular task according to their own learning needs. This accelerates user adoption, increases ROI on technology investments, and improves patient care outcomes. These tools also incorporate extensive AI and machine learning features that provide valuable insights that help leaders continuously improve training programs, workflows, and patient-facing applications.
Here are some of the most critical ways DAPs facilitate digital transformation:
1. Support Clinicians Navigating Complex, Multi-System Workflows
Mental health professionals often juggle multiple applications, such as EHRs, billing software, teletherapy platforms, and compliance tools. This complexity slows workflows, increases cognitive burden, and creates risk for errors that directly affect patient care. Digital transformation leaders in this space know that without integrated, intuitive support, adoption lags, and clinical efficiency declines.
Why it Matters:
- Documentation and consent errors introduce compliance risks.
- Siloed systems force clinicians into inefficient workarounds.
- High complexity leads to clinician frustration and burnout.
Whatfix in Action:
- Role-based guidance ensures a psychiatrist, therapist, or intake coordinator only sees support that matches their responsibilities.
- Embedded compliance prompts prevent incomplete or non-compliant forms before submission.
- Smart Tips surface clarifications inside workflows to reduce data-entry mistakes.
- Analytics reveal where clinicians struggle most, enabling leaders to refine both processes and training.

2. Accelerate Onboarding for EHR, Teletherapy, and Intake Portals
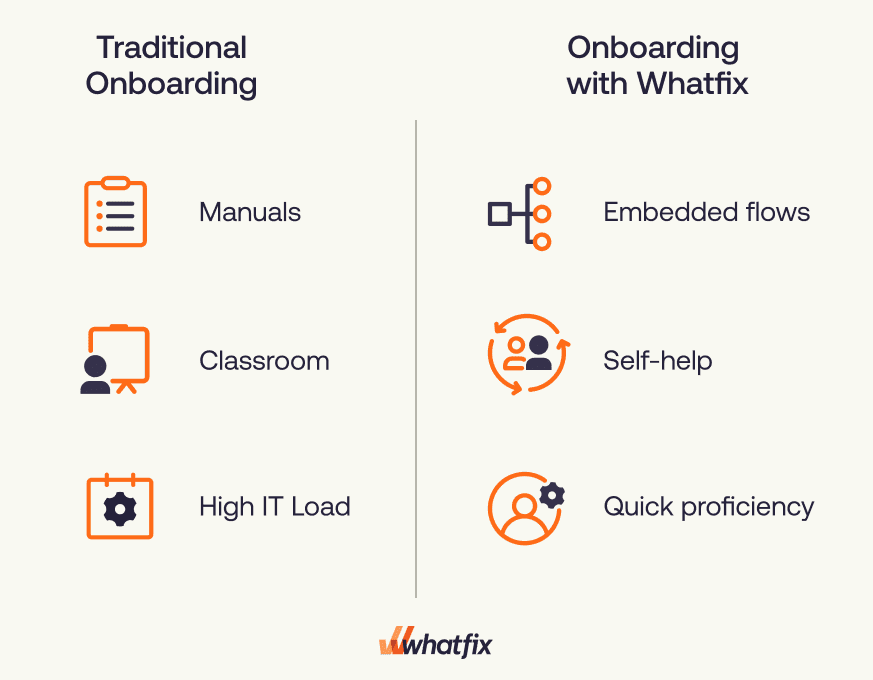
Traditional onboarding and training methods, such as lengthy manuals, slide decks, and classroom training sessions, don’t resonate with clinicians facing pressing patient demands. Mental health professionals need to learn in the context of real tasks, or adoption stalls, and support volumes spike. DAPs transform onboarding into resilient, embedded learning, making ramp-up faster and more intuitive.
Why it Matters:
- Clinicians forget training fast when not grounded in real workflows.
- Slow onboarding delays patient access and strains staff resources.
- IT/operations teams get overwhelmed by common support requests.
Whatfix in Action:
- Interactive Flows guiding new staff through documentation, scheduling, teletherapy setup.
- Self-Help panels inside systems to reduce support tickets.
- Tracking of task completion and proficiency by role or clinic.
- Contextual onboarding that replaces static training with in-system learning.
3. Empower Patients With Self-Guided Support Across Digital Tools
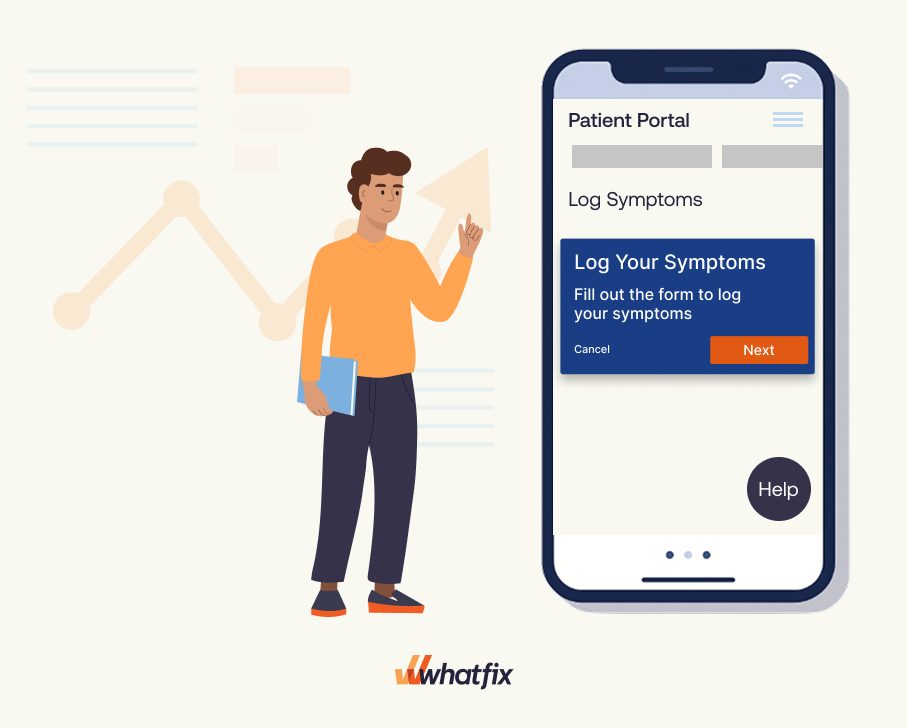
Completing forms, logging symptoms, and scheduling appointments—these digital actions become overwhelming when portals are poorly designed or unlabeled. Patients often abandon tools when they feel confused or inaccessible. DAPs help by surfacing contextual guidance, improving usability, and building confidence at every digital touchpoint.
Why it Matters:
- Confusing interfaces lead patients to avoid digital adoption.
- Increased support calls slow down operations.
- Poor digital experiences can erode trust.
Whatfix in Action:
- Interactive walkthroughs embedded in patient portals for tasks like appointment booking or symptom logging.
- On-page FAQs and Self-Help search that provide answers instantly.
- Low-intrusion design: help is available, not forced.
- Multi-language options and mobile-friendly flows for accessibility.
4. Deliver Scalable, Contextual Training Without Burning Out Staff
Clinicians already carry a heavy emotional load in their work. Requiring them to absorb lengthy manuals, attend repeated training sessions, or search through static documentation only adds to fatigue. Digital transformation leaders must ensure training is lightweight, contextual, and repeatable so adoption improves without creating additional stress.
Why it Matters:
- Training fatigue leads to disengagement and reversion to old processes.
- Repeated retraining requests overwhelm IT and operations teams.
- Burnout reduces both adoption rates and patient care quality.
Whatfix in Action:
- Microlearning in the flow of work that turns long SOPs into short, task-specific Flows.
- In-app guidance with nudges and reminders that appear exactly where errors or confusion are most likely.
- Always-available Self-Help with walkthroughs, policies, and FAQs in one central panel.
- Phased rollout support that delivers guidance by role or team during migrations to minimize disruption.
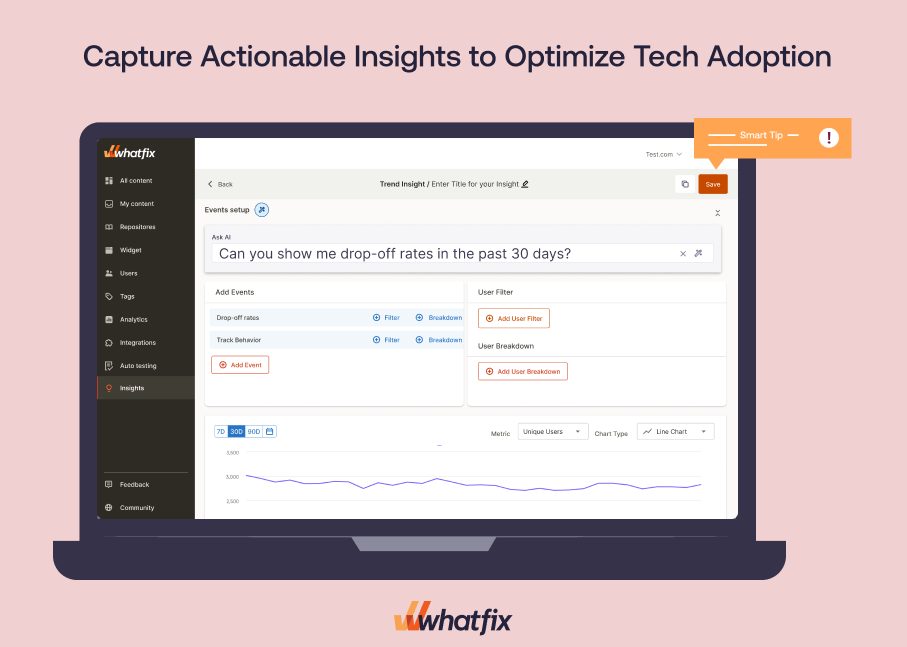
5. Capture Actionable Insights to Optimize Tech Adoption and Care Delivery
Launching a new system is only half the battle. Leaders need visibility into whether staff and patients use digital tools correctly, where they encounter friction, and which workflows fail to stick. Without analytics, it’s impossible to refine adoption strategies or prove ROI on technology investments.
Why it Matters:
- Lack of visibility means leaders can’t pinpoint adoption barriers.
- Without data, training programs remain reactive instead of proactive.
- Poorly understood workflows reduce efficiency and compromise care delivery.
Whatfix in Action:
- Analytics dashboards that track workflow completion rates, drop-offs, and errors.
- Step-level tracking to pinpoint where users abandon or struggle.
- Continuous improvement through quick updates to Flows at failing points with measurable impact.
- Correlation of adoption insights with help-desk data to prioritize fixes.
6. Standardize Digital Workflows Across Multi-Location or Hybrid Care Settings
Mental health organizations often operate across multiple clinics, hospitals, and telehealth hubs. Each location may have its own processes, which creates inconsistencies in documentation, billing, and reporting. Standardization is critical for quality and compliance, but it’s difficult to enforce without embedding protocols directly into staff’s tools.
Why it Matters:
- Variation in workflows undermines care consistency.
- Compliance gaps appear when SOPs differ across locations.
- Scaling transformation is nearly impossible without standardization.
Whatfix in Action:
- Master workflows cloned and adapted for local needs while maintaining consistency.
- Segmentation that delivers the right version of workflows by site, role, or specialty.
- Embedded SOPs that appear inside applications so users never leave their screen.
- Audit capabilities to monitor adherence and flag sites that deviate from protocols.

7. Drive Adoption of New Tools Without Disrupting Sensitive Clinical Environments
In mental health care, adoption strategies must protect the therapeutic relationship. Clinicians cannot afford to be distracted by clunky interfaces or disruptive training during live sessions. New tools must be introduced seamlessly so adoption strengthens patient care instead of undermining it.
Why it Matters:
- Visible friction during patient interactions erodes trust.
- Clinicians disengage if tools feel intrusive.
- Poorly managed rollouts compromise both adoption and care quality.
Whatfix in Action:
- Contextual, unobtrusive support that appears only when needed.
- Gradual adoption pathways piloted with champions and scaled across cohorts.
- Smooth migrations with side-by-side prompts mapping old workflows to new ones.
- Suppression of prompts in sensitive session views to protect therapeutic presence.

How AbleTo Achieves Its Digital Mental Care Vision With Whatfix
Leading virtual behavioral health provider AbleTo dramatically scaled its clinical team and improved care delivery with Whatfix. By embedding in-app guidance and analytics directly into the EnAbleTo platform, AbleTo was able to increase operational efficiency, reduce training dependencies, and deliver better patient and provider experiences.
The Challenge for Change Leaders
- In two years, AbleTo’s provider base expanded from around 200 to 2,000+ clinicians, vastly increasing the training burden. Maintaining care quality and supporting hundreds of new users became a major operational hurdle.
- Clinical meetings were consumed by support calls. 80% of team meeting time was spent on system-related issues, limiting focus on care improvement.
- Relying on live training and scattered documentation negatively impacted clinician experience and interrupted sessions, as providers frequently had to pause consultations to find help elsewhere.
What Did Whatfix Deliver?
AbleTo started a trial with Whatfix and discovered it was intuitive and unobtrusive—critical for preserving the therapeutic environment while adding support.
- Step-by-step onboarding experiences embedded in the application, enabling clinicians to learn directly in their workflow.
- Contextual walkthroughs and Smart Tips for self-support, available 24/7, easily searchable, and personalized.
- One specific health plan required providers to send reminder messages. AbleTo expected a 30% improvement in follow-through. Whatfix delivered a 50% uplift, enhancing compliance and care outcomes.
Real-World Outcomes for Digital Change Leaders
- Provider onboarding scaled 10x without additional overhead. AbleTo grew its provider base tenfold through efficient digital adoption.
- Saved $71,000 in just three months thanks to reduced search time and faster content creation.
- Patient task completion increased by 50%, signaling stronger engagement and fewer abandoned activities.
- Clinical meetings now 100% focused on clinical quality, compared to being 80% consumed by system support previously.
- Over 35,000 in-app pop-ups delivered, empowering clinicians and boosting productivity without manual intervention.
- Smart Tips viewed nearly 500,000 times across 18 guides, dramatically reducing support ticket volume.
- Whatfix has support baked into AbleTo’s upcoming Salesforce Health Cloud rollout, ensuring continuity and adoption across critical new platforms.
Why It Matters for CIOs and Change Leaders in Mental Health Services
For leaders building digital mental health infrastructure, the AbleTo case is a strong proof point:
- You can scale rapidly without burdening training teams.
- You improve clinician satisfaction, efficiency, and retention.
- You get measurable ROI through cost savings, productivity gains, and patient engagement.
- You accelerate adoption of new systems without compromising service quality.
Implementation Strategies for Mental Health Providers
Putting your digital transformation plan into action can be a complex and sensitive process, especially in the mental health field, where practitioners and the organizations they work for provide vital services to their patients.
As digital transformation becomes a reality for your mental health organization, follow these best practices to fast-track the successful implementation of your new technologies:
- Create a Transformation Roadmap Across People, Process, and Technology: Align goals for your transformation project across clinical operations, IT, and leadership to drive measurable outcomes and ensure continuity of care throughout the process.
- Select a Tech Stack that Supports Long-Term Scalability: Prioritize ease of integration and user-friendliness when choosing new software. Take things a step further by selecting platforms that pair well with DAPs to ensure maximum return on investment.
- Establish a Change Management Framework that Sticks: Drive adoption by communicating the value of each change early on. Do this by addressing sources of resistance and reinforcing new behaviors with in-app guidance.
- Equip Staff and Stakeholders With the Skills to Succeed: Deliver just-in-time learning, role-specific support, and structured onboarding to instill users with the confidence and competence necessary for successful adoption.
- Measure Impact through ROI and Outcome-Driven Metrics: Establish benchmarks and track KPIs throughout change implementation and tech rollouts. Include metrics like tool adoption rates, patient engagement, error reduction, and therapy adherence to evaluate success.
Mental Health Services Transformation Clicks Better with Whatfix
The future of mental health is digital, but transformation requires the right tools to enable patients and practitioners alike to optimize how they interact with healthcare technologies. Organizations that embrace adoption-first strategies will lead the way.
With Whatfix, mental healthcare leaders can accelerate digital adoption to improve service quality, provide patient-centric experiences, and streamline internal operations. From compliance training portals to EHR systems to appointment scheduling, Whatfix integrates with healthcare software to facilitate technology adoption and patient access to mental healthcare.
The Whatfix DAP integrates with all your essential healthcare apps to help employees adopt new software like telehealth platforms and EHR systems. Embedded support messages and helpful checklists support users as they navigate new workflows, expediting time-to-proficiency and building confidence with every takeaway.
Whatfix also helps providers support patients through the onboarding process, making it easier to establish care, schedule appointments, and attend virtual meetings without adding unnecessary stress to the mix. Whatfix Mirror allows developers to clone healthcare applications and test new workflows without risking security breaches or compliance issues.
Whatfix Product Analytics uses AI and real-time event tracking to help providers understand pain points for both patients and employees, and make data-informed decisions. With this tool, clinicians and other operational teams can measure the impact of digital transformation initiatives and continually improve user experience and overall mental health services.
Ready to learn more? Schedule your free demo today!