Since the 1980s, when electronic health record systems, known as EHR systems, went mainstream, they’ve seen massive adoption in developed economies. Most hospitals in countries like Australia (92%), New Zealand (97%), the United Kingdom (97%), and the Netherlands (98%) are being run electronically.
EHR systems are the foundation of modern healthcare operations, but investing in a platform is only step one of a transformation journey. True value realization happens when your healthcare organization goes beyond technical deployment to secure clinician engagement, sustainable use, and streamlined workflows.
However, EHR implementation remains challenging for modern healthcare organizations, with only 38% of healthcare leaders saying their implementations were successful, according to a recent 2025 Arch Collaborative report by KLAS Research. 75% of medical professionals say they’d benefit from additional EHR training and continued user support, highlighting a persistent gap between system deployment and real-world usability.
For CIOs and healthcare transformation leaders, the challenge isn’t deploying the EHR; it’s ensuring clinicians, front-office staff, and administrators adopt its full functionality and embed it into their daily workflows. Without a user-centric adoption strategy that invests in EHR training and support, healthcare IT and L&D teams can accelerate workflows, reduce support costs, unlock employee productivity, and realize the full potential of EHR systems and their advanced feature sets.
In this article, we’ll explore how to build a user-centric EHR implementation roadmap that focuses on end-user adoption and value realization, and share practical steps to ensure your project delivers on its potential, backed by strategy and solutions built for healthcare transformations.
What Is True EHR Implementation?
EHR implementation isn’t a one-time event. True implementation goes far beyond installing software or surviving the first go-live week. It’s a strategic, multi-phase journey that ensures clinicians and staff not only use the EHR but use it effectively, confidently, and in a way that meaningfully improves patient care.
Implementation ≠ Adoption
Installing an EHR and flipping the switch on go-live doesn’t guarantee success. True EHR implementation requires both technical readiness and human-centered change management. That includes user training, ongoing support, communication, and clear metrics.
Examples of Partial vs. Full Adoption
| Usage | A physician who logs in to enter vitals | A nurse who uses the EHR to document vitals |
| Adoption | A physician who uses clinical decision support tools to improve patient care | A nurse who understands how to chart more efficiently using templates and automations |
The goal of true EHR implementation is to move all users from surface-level functionality to full, confident, value-driven usage across the care continuum.
Key Phases of EHR Implementation
- Planning and assessment: This phase includes vendor evaluation, workflow analysis, infrastructure review, stakeholder alignment, and resource planning. At this stage, healthcare leaders must align clinical, IT, and administrative goals with the EHR system’s capabilities.
- System configuration and customization: EHRs need to reflect how care is actually delivered in each organization. Customization should support existing clinical workflows and not force workarounds. Mapping templates, alerts, and data fields to user needs is critical.
- Go-live and initial rollout: This is the moment the system moves from planning into daily use. It requires intense support, real-time troubleshooting, and embedded onboarding for staff. Many organizations mistakenly consider the job done here but this is only the start.
- Stabilization and support: In the weeks following go-live, organizations must shift from fire-fighting to supporting adoption. End-users need in-the-flow training and contextual support. Change fatigue, resistance, and productivity drops must be proactively managed.
- Long-term adoption and optimization: This is where true EHR value is unlocked. Organizations that continue investing in training, feedback loops, usage analytics, and workflow enhancements see sustained adoption and satisfaction. This phase ensures the EHR evolves with the organization’s needs and delivers ROI.
Core Barriers to EHR Implementation
Even with high EHR adoption rates, the implementation journey is fraught with pitfalls especially when it comes to ensuring systems are usable, sustainable, and embraced by end-users. Poorly executed implementations often lead to burnout, duplicative work, and costly inefficiencies that compound over time.
The chart below from the KLAS Arch Collaborative EHR Implementations 2025 Report highlights the top barriers as reported by healthcare organizations:
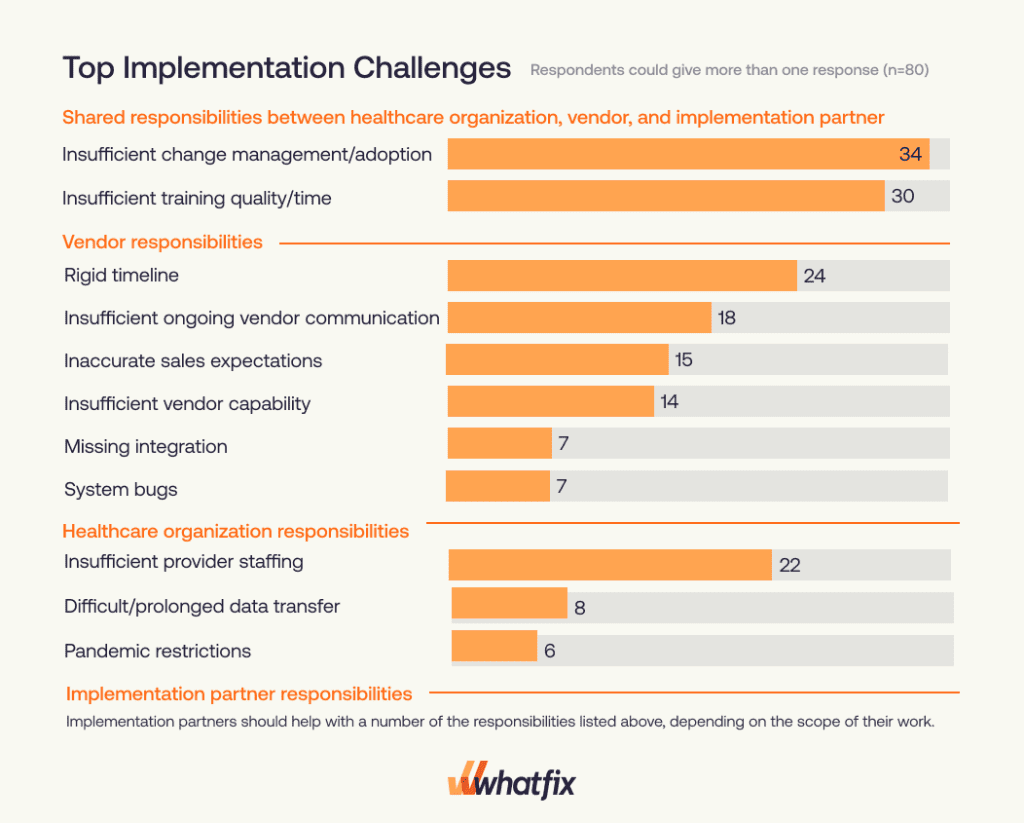
Let’s explore these and additional barriers that contribute to failed or suboptimal EHR rollouts:
- Insufficient change management and end-user adoption: According to KLAS, 34% of organizations cite change management and adoption issues as the top shared barrier between vendors, implementation partners, and healthcare organizations. Without leadership alignment, clinician buy-in, and end-user engagement, new systems are seen as burdens, not enablers. Becker’s Hospital Review also flags this as the most cited implementation failure point.
- Inadequate training time and quality: 30% of organizations report training as a key challenge. Most training is rushed, overly generic, or disconnected from real workflows. This leads to poor user confidence, increased errors, and long ramp-up periods that ultimately delay true adoption.
- Rigid timelines and poor vendor coordination: Vendors pushing rigid go-live timelines without adequate readiness create major risks. Additionally, 24% cite lack of ongoing vendor communication as a top issue. When vendors and implementation partners don’t collaborate effectively, organizations are left to bridge the gap.
- Technology usability and workflow fit: Even after implementation, usability friction, poor UX, and fragmented integrations between EHRs and other clinical systems create frustration. Clinicians struggle with clunky interfaces, redundant data entry, and inefficient navigation paths that increase cognitive load. Studies show this can increase documentation time by 11–22%, contributing to burnout.
- Resource constraints and staffing gaps: Nearly a quarter (22%) of healthcare organizations cite insufficient provider staffing as a top implementation challenge. Many hospitals, especially rural and mid-size systems, lack the bandwidth to dedicate full-time resources for configuration, training, and support.
- Poor data migration and system integration: Mismatched legacy data, prolonged transfers, and missing integration points add complexity. When data is siloed or inaccurate post-migration, clinician trust in the system drops and reliance on paper or shadow workflows increases.
- Limited visibility into implementation progress: Without behavioral analytics, teams can’t track where users are struggling, what features go unused, or how workflows are breaking down. This invisibility hinders early interventions, prolongs stabilization, and prevents long-term optimization.
Why User Adoption Is Key to EHR Value Realization
Adoption doesn’t end when your EHR system goes live. True EHR adoption means that every end-user (clinicians, nurses, administrative staff, billing teams) uses the system effectively, consistently, and as intended to improve patient care, operational efficiency, and data accuracy.
Many healthcare organizations confuse implementation with adoption. But rolling out software and training a few super users isn’t enough to create lasting change. Even well-planned go-lives can falter without sustained support. Clinicians may struggle with clunky interfaces. Front-desk staff may skip steps. Nurses may rely on paper workarounds. This isn’t a usability problem; it’s an adoption failure. Without clear training, workflow alignment, and change management, partial adoption becomes the norm. For example:
A hospital might implement an EHR with patient portal functionality but see less than 10% of patients use it due to staff not promoting it or workflows not incorporating it. Or a billing team might enter data inconsistently, leading to coding errors and delayed reimbursements not because they’re unwilling, but because the EHR workflows weren’t intuitive or well-trained.
For CIOs and transformation teams, under-adoption is a hidden cost that shows up as increased support tickets, clinician burnout, poor data quality, and stalled performance metrics. Realizing ROI from your EHR investment requires moving beyond go-live to ensure deep, lasting adoption across all user types.
Common Barriers To EHR Adoption
Despite wide-scale implementation, many healthcare organizations struggle to reach full EHR adoption. Below are six common blockers that limit EHR effectiveness, frustrate end-users, and stall digital transformation.
- Usability friction and cognitive load: Modern EHR systems are powerful but also complex. Clinical staff often juggle dozens of tasks across different modules, screens, and alerts. Without streamlined workflows and intuitive navigation, EHRs can overwhelm users, especially in high-pressure care settings. This leads to errors, workarounds, and slower task completion. This friction directly impacts care quality and efficiency and undermines the promise of digital transformation.
- Training gaps and one-time onboarding: Most organizations invest in upfront training but fail to support users beyond the go-live window. One-size-fits-all LMS modules or classroom sessions aren’t sufficient for long-term adoption, especially when systems evolve post-implementation. Clinicians quickly forget workflows they don’t use often. New staff enter without formal onboarding. The result: reliance on peers, inconsistent usage, and rising support requests.
- Lack of in-workflow support: When clinicians or administrative staff get stuck, help is often far away buried in static documentation, siloed in a separate knowledge base, or locked behind helpdesk queues. This disconnect slows users down and forces them to abandon digital workflows. Without real-time, contextual support, adoption becomes fragile. Users will revert to paper, external tools, or incorrect shortcuts when digital workflows fail them in the moment of need.
- Resistance to change: Healthcare professionals are highly specialized and time-constrained. Introducing new digital workflows without involving frontline users or addressing their concerns often leads to pushback. Some fear loss of control. Others question the value or necessity of new systems. Without buy-in, even the best-designed EHR deployments can see limited adoption across departments.
- Ineffective communication: New workflows, system upgrades, or compliance changes are often communicated through emails or generic intranet updates. These channels that are easily overlooked by busy healthcare teams. When users aren’t informed at the right time, in the right context, rollout momentum slows. Misinformation spreads. And training efforts go underutilized.
- Limited visibility into adoption metrics: Most EHR platforms offer basic activity logs, but they lack the granularity to reveal where users are dropping off, skipping steps, or misusing features. This leaves transformation teams guessing which workflows need support or where to intervene to improve outcomes. A lack of actionable adoption data means strategy decisions are based on assumptions, not insight.
Building an Effective EHR Adoption Strategy With Whatfix
Adopting an EHR system isn’t a one-time implementation task, it’s a continuous journey of improving usability, driving behavior change, and supporting frontline staff across the entire lifecycle of the system. To realize the system’s value at scale, healthcare organizations must go beyond one-time onboarding and embrace a system of in-workflow enablement, personalized learning, and real-time support.
Here are six key components of a successful EHR adoption strategy and how Whatfix helps drive outcomes in each area.
1. Pre-Go-Live Testing and Simulation
Rushing from EHR configuration to go-live without validating workflows can create major risks, from user confusion to compliance issues. Testing how different roles experience core workflows ensures adoption isn’t derailed by overlooked friction points.
How Whatfix Helps:
Whatfix Mirror allows IT and clinical informatics teams to replicate EHR environments like Epic, Cerner, or MEDITECH in a secure sandbox. These simulated training environments are ideal for validating configurations, conducting role-based testing, and training users in a risk-free space without touching production data.
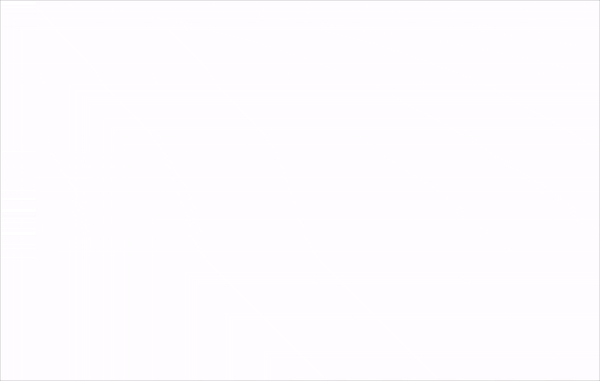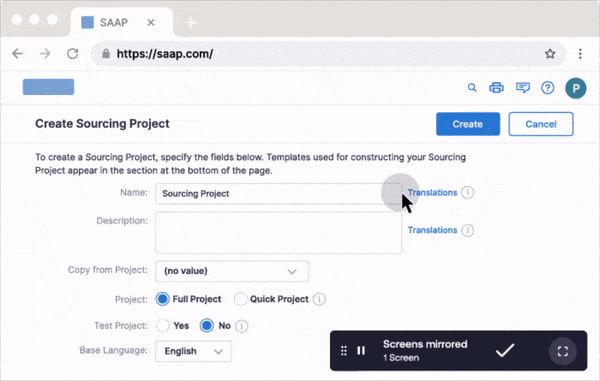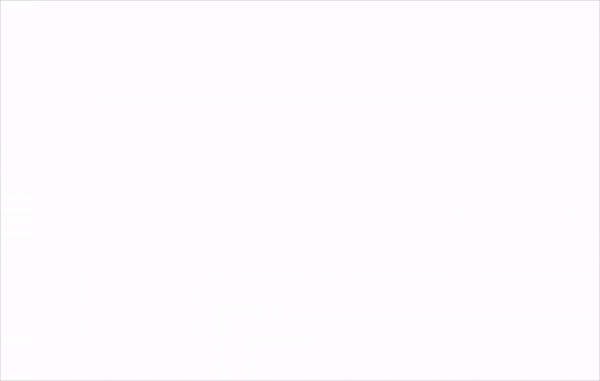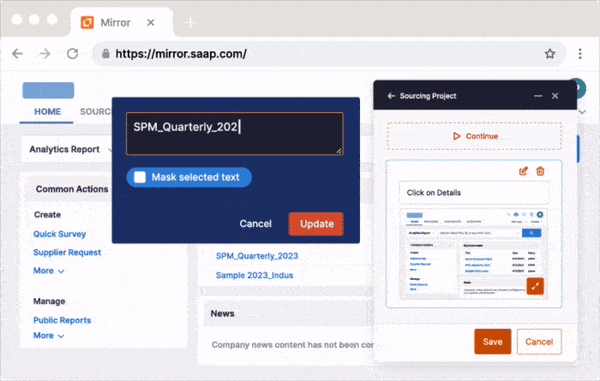
2. Role-Based Onboarding for Clinicians and Staff
Generic training modules often fail to meet the needs of clinicians, nurses, and front-office staff who each use the EHR differently. Personalized onboarding is essential for faster time-to-productivity and higher user confidence.
How Whatfix Helps:
Whatfix delivers in-app onboarding tailored by user role, specialty, or location. With contextual task lists and walkthroughs embedded directly into the EHR interface, users are guided through real tasks like charting, e-prescribing, coding, as they perform them. This helps eliminate the learning curve and reducing help desk dependency.
3. Embedded Support in the Flow of Care
Busy clinicians and staff don’t have time to consult manuals or wait for IT when they’re stuck. Without real-time help, users revert to unsafe workarounds or skip critical steps entirely.
How Whatfix Helps:
With Whatfix Self Help, contextual support is available instantly, directly within the EHR interface. Users can access walkthroughs, troubleshooting tips, or clinical policy content without switching systems. This reduces support tickets and empowers users to solve problems in the moment.
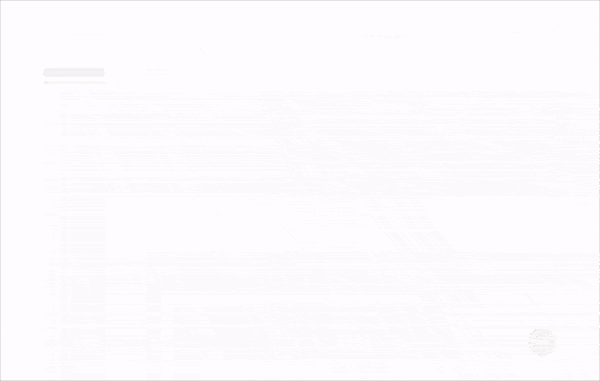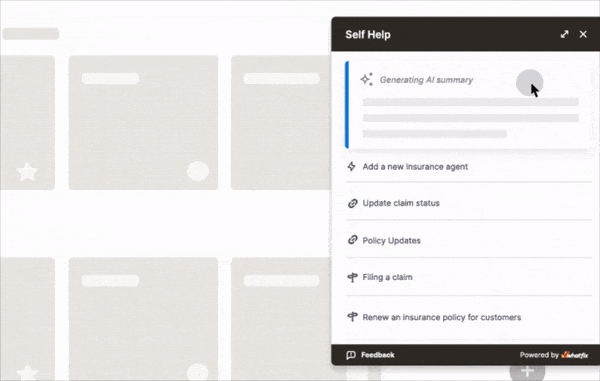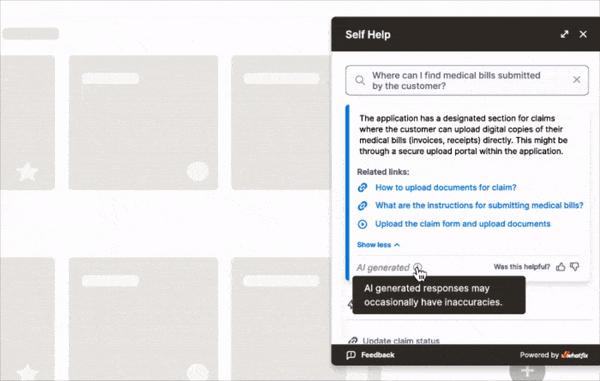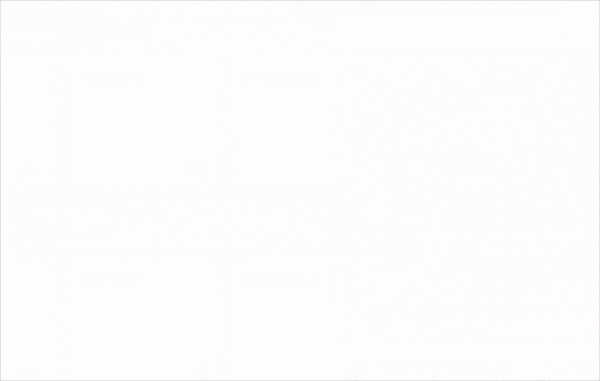
4. Communicating Policy & Workflow Changes in Real-Time
Whether it’s a new clinical protocol, billing update, or system enhancement, healthcare organizations frequently change their EHR workflows. But when change communication is siloed in email or the LMS, it’s often missed. This leads to non-compliance and process gaps.
How Whatfix Helps:
Whatfix allows IT and clinical training teams to deliver change alerts via in-app Pop-ups, Beacons, and Smart Tips. Whether announcing a new discharge workflow or documenting changes to medication reconciliation, Whatfix ensures users see and act on updates when they’re most relevant.
5. Increasing Adoption of Underutilized EHR Features
Many users only engage with core EHR features and ignore high-value capabilities like care coordination, health information exchange (HIE), or decision support tools. This underutilization stalls transformation and ROI.
How Whatfix Helps:
Whatfix nudges users to explore underused features through contextual prompts and proactive onboarding. With analytics, IT teams can identify where adoption is lagging and deploy targeted walkthroughs or support to guide users toward advanced functionality.
6. Measuring and Optimizing EHR Adoption
Without behavioral insights, it’s hard to know where workflows are breaking down or which users are struggling. Traditional EHR reporting tools offer limited visibility into user behavior at a task level.
How Whatfix Helps:
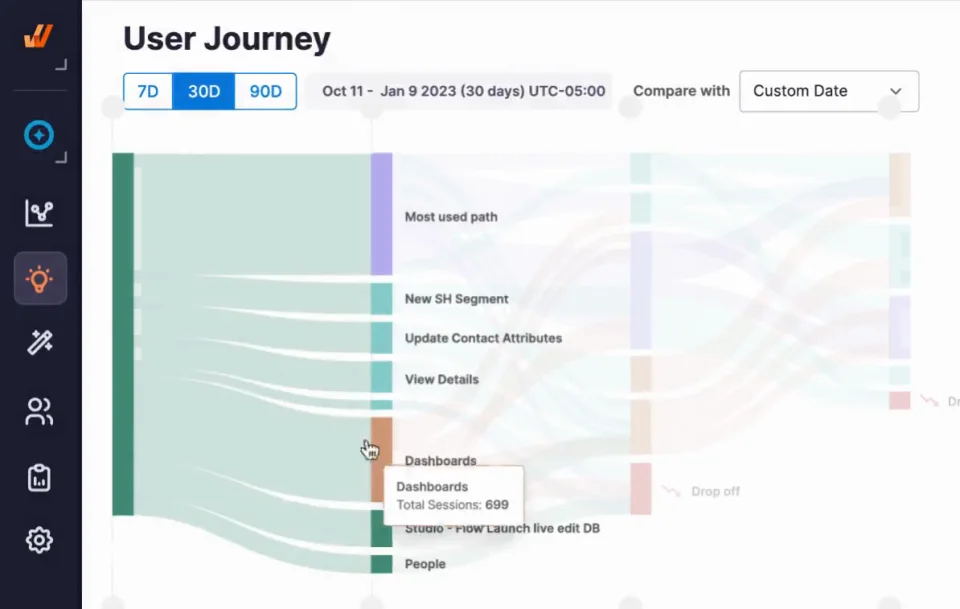
Whatfix Product Analytics tracks how users interact with EHR workflows in real time. IT and informatics teams can identify drop-offs, inefficient paths, or misused features then rapidly intervene with guided Flows or updated training to improve usability and performance.
Frequently Asked Questions (FAQs)
How long does full EHR adoption take?
Full EHR adoption is not a one-time milestone, it’s a continuous journey. While go-live might be achieved in a matter of weeks or months, meaningful adoption that drives efficiency, accuracy, and satisfaction often takes 6–12 months or more. The timeline depends on factors like user readiness, training quality, EHR usability, and post-launch support. Sustained adoption requires ongoing enablement, feedback loops, and system optimization.
What’s the best way to train physicians on a new EHR system?
For physicians, time is scarce and workflows are complex so training must be fast, relevant, and embedded in real tasks. Best practices include:
- Role-based, in-app onboarding tailored to clinical workflows
- Simulation environments for risk-free hands-on practice
- Contextual support during tasks to reinforce learning without slowing down care
- Peer champions to model behavior and answer real-world questions
Can you track how well employees are adopting the EHR?
Yes. Adoption success isn’t just about logins or time spent in the system, it’s about task completion, error rates, and confidence. With a DAP like Whatfix, you can:
- Track task-level engagement and drop-offs
- Segment data by role, location, or department
- Measure time-to-proficiency and usage of high-value features
- Use insights to refine training and provide targeted support
This data-driven approach helps healthcare IT leaders continuously improve adoption and prove ROI to stakeholders.
How do you provide EHR training without disrupting care delivery?
Traditional classroom sessions and LMS modules often pull clinicians away from patient care. Instead, modern strategies focus on in-the-flow-of-work learning where training is delivered directly inside the EHR, during actual tasks.
Whatfix enables this with:
- Step-by-step walkthroughs for real-time guidance
- Smart Tips and Self Help embedded in clinical workflows
- Sandbox environments for hands-on training without affecting live data
This approach minimizes disruption, builds confidence, and ensures that training happens where it’s most effective, at the point of care.
Software Clicks Better With Whatfix
Whatfix empowers healthcare organizations to accelerate EHR adoption and improve end-user performance with personalized, in-app guidance and real-time support.
From onboarding and workflow training to change communication and self-service support, Whatfix helps your teams get the most from your EHR investment without pulling them away from patient care.
With built-in analytics, you can track how users engage with the system, identify friction points, and continuously improve adoption across roles and locations.
See how Whatfix helps healthcare IT teams deliver better EHR outcomes, schedule a personalized demo with us today!